What is Arthritis?
Arthritis is a general term covering numerous conditions where the joint surface (cartilage) wears out. The joint surface is covered by a smooth articular surface that allows pain free movement in the joint.
When the articular cartilage wears out, the bone ends rub on one another and cause pain. There are numerous conditions that can cause arthritis and often the exact cause is never known. In general, but not always it affects people as they get older (Osteoarthritis).
In an Arthritic Knee
- The cartilage lining is thinner than normal or completely absent. The degree of cartilage damage and inflammation varies with the type and stage of arthritis
- The capsule of the arthritic knee is swollen
- The joint space is narrowed and irregular in outline; this can be seen in an X-ray image
- Bone spurs or excessive bone can also build up around the edges of the joint
The combinations of these factors make the arthritic knee stiff and limit activities due to pain or fatigue.
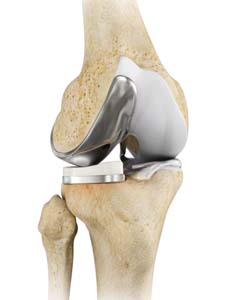
What is Unicondylar Knee Replacement
Unicondylar knee replacement simply means that only a part of the knee joint is replaced through a smaller incision than would normally be used for a total knee replacement.
Total knee replacement surgery replaces the ends of the femur (thighbone) and tibia (shinbone) with plastic inserted between them and usually the patella (kneecap).
Indications for Unicondylar Knee Replacement
The indications for unicondylar knee replacement include:
- Ideally should be over 50 years of age
- When pain and restricted mobility interferes with your lifestyle
- One compartment involved clinically and confirmed on X-ray
You may not be suitable for unicondylar knee replacement in the following cases:
- Arthritis affects more than one compartment
- Severe angular deformity
- Inflammatory arthritis e.g. rheumatoid arthritis
- Unstable knee
- Previous osteotomy
- You are involved in heavy work or contact sports
Preparation for Unicondylar Knee Replacement
Before surgery, your surgeon will send you for routine blood tests and any other investigations required prior to your surgery. You should have any other medical, surgical or dental problems attended to prior to your surgery. Make arrangements for help around the house prior to surgery. Cease aspirin or anti-inflammatory medications 10 days prior to surgery as they can cause bleeding. Cease any naturopathic or herbal medications 10 days before surgery. Stop smoking as long as possible prior to surgery.
Unicondylar Knee Replacement Procedure
Each knee is individual and knee replacements take this into account by having different sizes for your knee. If there is more than the usual amount of bone loss, sometimes extra pieces of metal or bone are added.
Surgery is performed under sterile conditions in the operating room under spinal or general anesthesia. You will be on your back and a tourniquet applied to your upper thigh to reduce blood loss. Surgery will take approximately two hours. You will be positioned on the operating table and your leg prepped and draped. A tourniquet is applied to the upper thigh and the leg is prepared for the surgery with a sterilizing solution.
An incision around 7cm is made to expose the knee joint. The bone ends of the femur and tibia are prepared using a saw or a burr. Trial components are then inserted to make sure they fit properly. The real components (femoral and tibial) are then placed with or without cement. The knee is then carefully closed and drains usually inserted, and the knee dressed and bandaged.
Post-operation Course for Unicondylar Knee Replacement
When you wake, you will be in the recovery room with intravenous drips in your arm, a tube (catheter) in your bladder and a number of other monitors to check your vital observations. You will usually have a button to press for pain medication called a PCA machine (patient-controlled analgesia).
Once stable, you will be taken to the ward. The post-op protocol is surgeon dependent, but in general, your drain will come out at 24 hours and you will sit out of bed and start moving you knee and walking on it within a day or two of surgery. To avoid lung congestion, it is important to breathe deeply and cough up any phlegm you may have.
Usually you will remain in the hospital for 3-5 days. Depending on your needs, you will then return home or proceed to a rehabilitation facility. You will need physical therapy on your knee following surgery. You will be discharged on a walker or crutches and usually progress to a cane at six weeks. Your sutures are sometimes dissolvable but if not, are removed at approximately 10 days.
Bending your knee is variable, but by 6 weeks, it should bend to 90 degrees. The goal is to obtain 110-115 degrees of movement. Once the wound is healed, you may shower. You can drive at about 6 weeks, once you have regained control of your leg. You should be walking reasonably comfortably by 6 weeks. More physical activities, such as sports previously discussed may take 3 months to be able to do comfortably.
You will usually have a 6 week check up with your surgeon, who will assess your progress. You should continue to see your surgeon for the rest of your life to check your knee and take X-rays. This is important as sometimes, your knee can feel excellent, but there can be a problem only recognized on the X-ray.
If you have any unexplained pain, swelling, or redness or if you feel generally poor, you should see your doctor as soon as possible.
Advantages and Disadvantages of Unicondylar Knee Replacement
The decision to proceed with knee replacement surgery is a cooperative one between you, your surgeon, family and your local doctor.
The benefits following surgery are relief from arthritic pain, stiffness and deformity - either bowleg or knock knees. Other advantages include
- Smaller operation
- Smaller incision
- Not as much bone removed
- Shorter hospital stay
- Shorter recovery period
- Blood transfusion rarely required
- Better movement in the knee
- Feels more like a normal knee
- Less need for physiotherapy
- Able to be more active than after a total knee replacement
The big advantage is that if for some reason it is not successful or fails many years down the track, it can be revised to a total knee replacement without difficulty.
However, unicondylar knee replacement is not quite as reliable as a total knee replacement in relieving pain and the long-term results are not quite as good as total knee.
Risks and Complications of Unicondylar Knee Replacement
As with any major surgery, there are potential risks involved. The decision to proceed with the surgery is made because the advantages of surgery outweigh the potential disadvantages.
It is important that you are informed of these risks before the surgery takes place.
Complications can be medical (general) or local complications specific to the knee
Medical complications include those of the anesthetic and your general well-being. Almost any medical condition can occur, so this list is not complete. Complications include:
- Allergic reactions to medications
- Blood loss requiring transfusion with its low risk of disease transmission
- Heart attacks, strokes, kidney failure, pneumonia, bladder infections
- Complications from nerve blocks such as infection or nerve damage
- Infection
- blood clots (deep venous thrombosis)
- Fractures
- Stiffness in the knee
- Wearing of the prosthesis
- Wound irritation
- Leg-length inequality
- Dislocation
- Damage to nerves and blood vessels